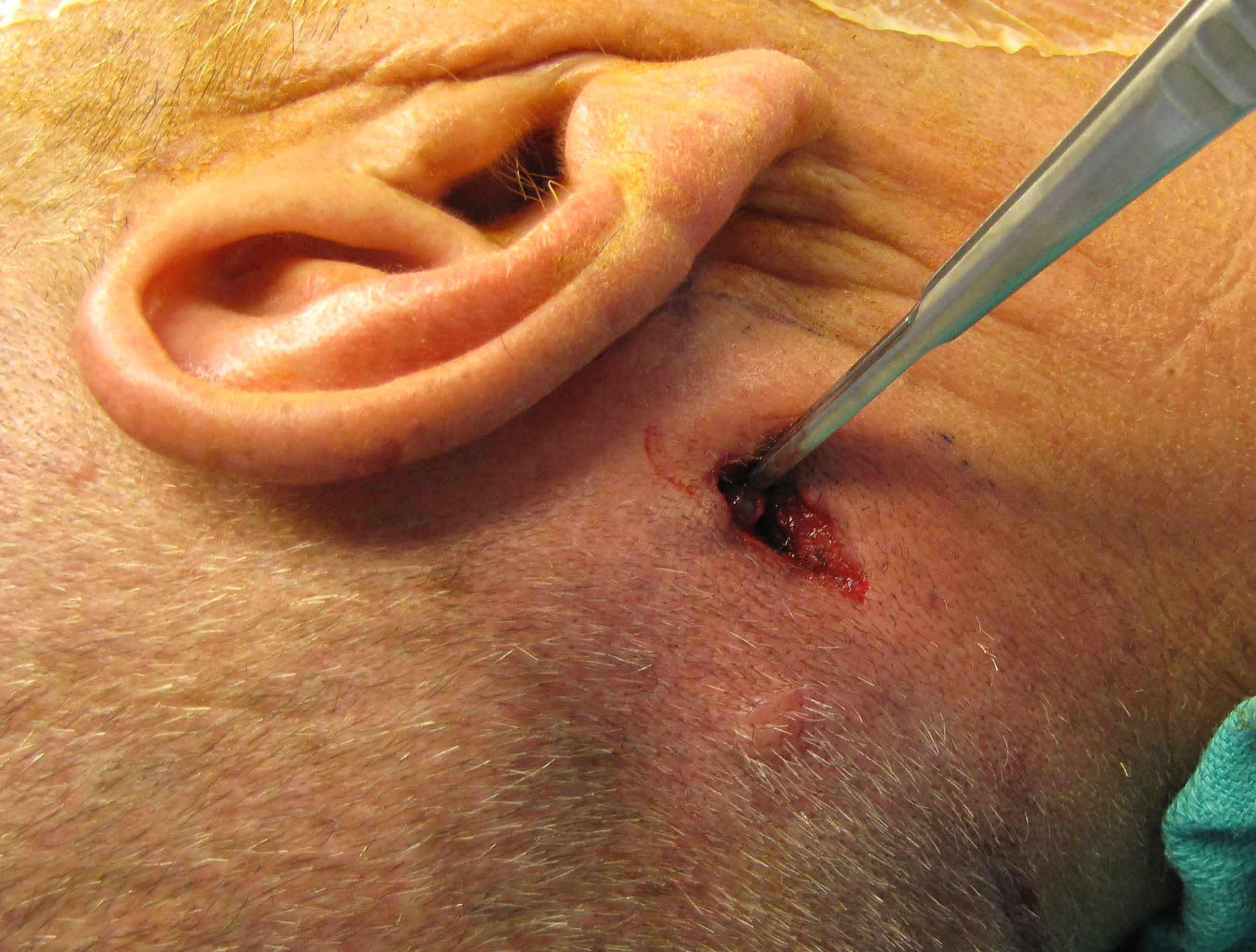
To reduce the potential side effects, the BD are routinely diluted with normal saline (practices vary from 1:1 to 1:7 dilution) ( 17).
#Sentinel node skin#
MB has a reduced risk of anaphylaxis but showed side effects as well ( 14, 15): skin necrosis and induration with associated pain, up to pulmonary edema and serotonin syndrome in patients who take serotonergic medications ( 16). In case of isosulfan blue it has been reported in 0.7% to 1.1% of cases ( 12, 13). Indeed one of the major problem of BD is a possible adverse reaction up to an anaphylaxis. Each surgeon should look for the method that works best for his or her practice, even though isosulfan and patent blue seem to cause a higher rate of adverse reactions ( 11). Three types of BD have been described: isosulfan blue, methylene blue (MB) and patent blue. ( 10) accurately described best practices for both of these tracers besides to the main problems linked to them. reported a 82% SLN identification rate using only RI and gamma probe. reported a 93% SLN identification rate using BD alone, while Krag et al. ( 3) have been developed both as single technique and as dual complementary procedure: the choice is determined by surgeon and institutional preference. The traditional SLNB techniques proposed by Giuliano et al. This paper is a comprehensive review of the currently used techniques for SLNB with a specific focus on the new innovative ones.Ĭurrent standard of care for SLNB-blue dye and/or technetium labelled nanocolloid Clinical trials demonstrated that in these kinds of patients a properly performed SLNB is equivalent to axillary lymph node dissection (ALND) for staging of axilla ( 6- 8), identifying patients who need further axillary clearance, while sparing others a potentially morbid ALND ( 9). SNB has since become the new standard of care for axillary staging in clinically and radiologically node-negative BC ( 5). described the SNB using BD alone as a procedure technically feasible, safe, and highly accurate to stage regional LNs in BC ( 4). described and developed the gamma probe localization of SLN with RI Giuliano et al. SLNB, as ideal nodal staging method for BC, was introduced by Krag et al. SLN status accurately predicts the status of the other LNs and is important to establish staging and prognostic outcomes of BC. Locoregional spread of breast cancer (BC) occurs mainly through the lymphatic system. identify lymphatic drainage patterns of melanomas and the development of SLNB technique through intraoperative lymphatic mapping ( 1). The advent of percutaneous lymphoscintigraphy allowed Robinson et al. Therefore, SLN is defined as the first LN that receive lymphatic drainage from the primary tumour, if the tumour has spread. Accepted for publication Feb 01, 2018.Īccording to sentinel lymph node (SLN) hypothesis, tumor cells migrate in an orderly manner from a primary tumour, metastasizing to one or a few LNs before involving others. Keywords: Breast cancer (BC) sentinel node biopsy indocyanine green (ICG) superparamagnetic iron oxyde microbubble This is a comprehensive review of current limitations of conventional techniques besides the improvements and innovations of new methods which, anyway, need future randomized controlled trials to be fully validated. Whilst each technique has its own advantages/disadvantages they are increasing their efficacy and are candidate to represent a new standard for SLNB in next future. Because of several drawbacks reported in worldwide experiences, new techniques have been developed in the last years: indocyanine green (ICG) fluorescence, superparamagnetic iron oxide (SPIO) nanoparticles and contrast-enhanced ultrasound (CEUS) using microbubbles.
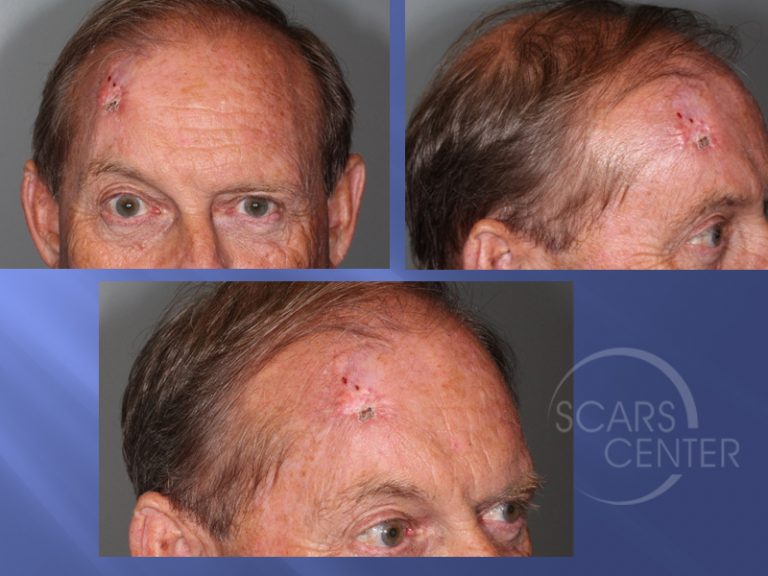
The actual standard for SLNB is the radioisotope (RI) with or without blue dye (BD) technique. It successfully replaced the more invasive and morbid axillary lymph node dissection (ALND). Abstract: Sentinel lymph node biopsy (SLNB) is still the standard of care for axillary nodal staging in patients with invasive breast cancer (BC) and clinically negative lymph nodes (LNs).
